
|
|
|
Next | ||
RBRVS Payment screens |
||||
|
|
||||
1. Just click on the dollar value in order to see additional detailed information for the code.
Having done this, the Payment screen detail come into view. This looks imposing, but we'll dissect it into bite sized amounts.

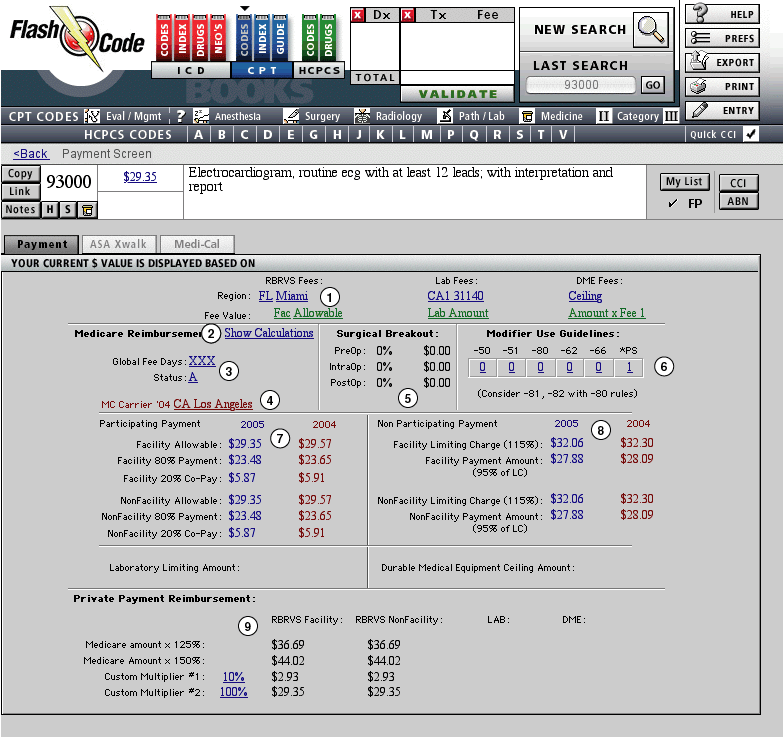
2. The Show Calculations link will take you to the actual RBRVS calculation. It will display the work, malpractice, and practice expense RVUs, their corresponding Geographic Practice Cost Index (GPCIs), and the current Conversion Factor (CF) as set by congress. View Example
3. For most surgical procedures, medicare sets a time period during which any care is covered by the global surgical package payment amount. Most are 10, 30, or 90 days, but others have letters that signify other meanings. Click the link next to the Global Fee Days to see the description of these meanings.
4. Flash Code includes the fee tables for current data and one year old data. The medicare carrier can be changed to see differences in fees across the nation, or to compare lasts year's fee with the current year.
5. Medicare presents a breakdown of the global surgical fee package into three component parts:
-Preoperative workup
-Intraoperative procedure
-Postoperative care
This breakout is of particular interest to surgeons who need to determine how to divide procedures where different portions of the procedure are done by different surgeons.
6. Medicare provides a listing of modifier rules for the codes covered under the RBRVS system. Each modifier contains a number that correlates to a key that further describes modifier rules for that code. Click the link to see whether a modifier can be billed, if documentation must be submitted, etc.
7. Medicare participating physicians receive payment directly from medicare for services provided. As such, they accept Medicares Allowable Amount, less the 20% patient co-pay. This amount can be billed to the patient at the time of service, or send off to a secondary insurance carrier.
-Services performed in a Facility include hospitals, ambulatory surgery centers, and skilled nursing facilities
-Everything else is considered to be a nonFacility.
Note that the reimbursement for nonFacilities is greater since the provider is also paying for the expense of the office in which the service was provided. Facilities bill separately for their portion of services provided, absorb the cost of overhead, therefore the physician payment is lower.
8. Nonparticipating physicians get to bill 115% of the usual Medical Allowable Amount. Medicare then pays 95% of that amount. However, payment from medicare is made to the patient. It is the responsibility of the provider's billing team to collect payment from the patient.
9. Flash Code automatically calculates a medicare amount x 125% and 150%. These values are displayed for informational purposes only. Users can also set additional percentage amounts to view as part of their fee creation or selection process.